My son, Matt, is a cyborg! Okay, not in the Borg sense, but he certainly has little machines on his body that communicate with little computers. Why does my son sound like he belongs on Star Trek and not our little Pacific Northwest home?
He is Type 1 Diabetic.
First, I want to say I am not a doctor nor a medical professional. This is just my son’s story. Like many parts of my family’s life, and this 20-murder-hornet-monkey-blood-stealing-dinosaurs-are-next-masks-aren’t-for-villains-20, I try to retain a sense of humor. If you think you or a loved one may have Type 1 Diabetes or any other illness, you should contact a medical professional immediately.
Shortly before Matt’s 10th birthday and Halloween in 2019 we received a phone call after a routine checkup asking us to check Matt into the hospital as soon as possible. His blood glucose was over 500 and he had ketones in his urine. As a parent, I didn’t know what any of that meant at the time, but I was terrified. We complied and raced to pick Matt up from school as calmly as possible and explained what we could to him while driving to the hospital.
Matt was lucky. He only spent a couple of days in the hospital. Other people aren’t as lucky.
Diabetes is an autoimmune disease. The geoduck-shaped organ, the pancreas, produces insulin in normal people. In Type 1 Diabetics it puts out its “Closed for Business: Retired” sign and sits drinking afternoon cocktails, taking up space in the body, and doing little else—especially not producing insulin. When this happens, the lack of insulin production creates problems like high blood glucose. This leads to a long list of other health problems. It also, over time, creates acidic blood or ketones, which still makes me think my son is somehow related to the aliens in the popular franchise. Thankfully, his blood has not turned glowstick green. Have I mentioned it is important to keep a sense of humor when you have a child with a chronic condition?
Type 1 Diabetes is not caused by eating too much sugar. It is not preventable. It is genetic. It can be diagnosed in any person at any age. There have even been genetic studies to find genetic markers indicating the likelihood of having Type 1 Diabetes. Matt actually was part of a study when he was born that indicated he had those markers that put him at higher risk. If someone you know has Type 1 Diabetes, they can eat whatever they want as long as they have insulin administered too. Also, please, with sugar and cream, on top do not think for a second that cinnamon cures diabetes. Just please don’t.
What did we see that made us wonder if he was diabetic?
- Constant thirst
- Needing to urinate frequently
- Weight loss
- Upset stomach (was even tested for celiac)
- Migraines
- Constant hunger (think if two 14-year-old boys shared the same body)
Fast forward a year. Matt has been through the process of grieving the loss of his pancreas (even though it is still in his body). He has learned how to check his blood glucose levels, knows when his blood sugar is high, and has pretty good multiplication skills from figuring out how many units of insulin he needs to take based on how many carbs he is going to eat. He has become well acquainted with the measuring cups and spoons, so he knows how much of a food he is eating and can accurately determine how many carbs are in that portion. Much of this process is made much simpler with technology.
The simplest tools a diabetic uses are a Blood Glucose Meter and insulin injections. Ultimately, every time a diabetic wants to consume carbohydrates, they stick a finger with a tiny needle to get a blood sample to indicate their blood glucose level. Then, they figure out based on their personal ratios how many units of insulin need to be administered through an injection. The goal is to keep their blood glucose levels in range. Too high for a long time is bad; too low for a short time is very bad. This process happened for us 3-6 times a day.

A Continuous Glucose-Monitoring Device, or CGM, is a little transmitter that is injected into the skin approximately once a week depending on which system is used. The purpose of this device is to give real-time, constant readings of an individual’s blood glucose levels. When levels are too high or low, an alarm on a phone or synced device sounds so the problem can be handled. For our son, this means most of the time he can check his phone for his current blood sugar instead of poking his finger and putting blood on a little strip. Because he has it set up on a phone, dad and I can “follow” his levels on our own phones and also get alarms—even when he is at school and we are at work. Plus, he can decorate it with stickers!
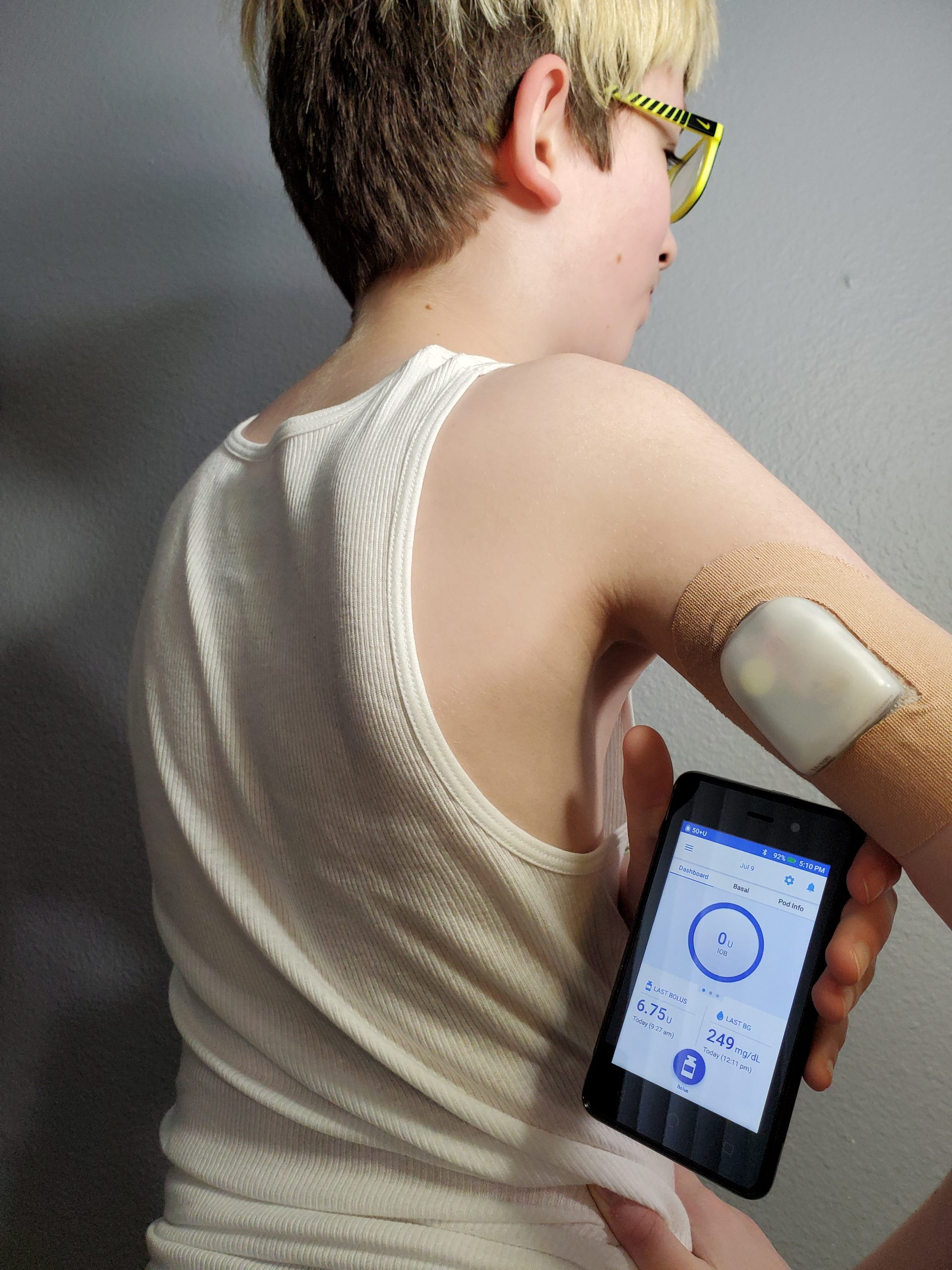
An Insulin Pump is another nifty device that helps imitate a pancreas. This device, depending on which one is used, is attached to the skin and has a little IV tube that goes into the skin. When the user tells it with a device how many carbohydrates are going to be consumed and their current blood glucose, the little device gives insulin. For Matt, this means he can wear the device and eat when he wants without needing to consider if he wants to endure an injection for the third breakfast he is eating due to a growth spurt. (He’s 10 and 5′ 1″—I know he will eat more than this in a few years.)
These devices can even work together. In very specific marriages between CGMs and pumps, the two can communicate and correct blood sugar that is predicted to be too high or low minutes into the future. All of this technology is amazing and makes life much less complicated and confusing considering Matt’s pancreas thought it would be great to take early retirement.
All this being said, there are huge costs associated with these devices. Not all diabetics can afford them, let alone the insulin they need to live. There are other complications and illnesses that can be associated with Diabetes. Exercise, a common cold, growing, puberty, and stress all play a part in what an individual’s blood glucose will decide to be. It isn’t just measuring food and taking the correct amount of insulin for that food. It’s stressful.
There are many celebrity Type 1 Diabetics out there. The one who I see mentioned regularly is Nick Jonas. Other celebrities range from American Idol contestants, athletes, television chefs, and stage/screen actors.
Some of my favorite geek diabetics include a gamer who started a stream that celebrates life and gaming and strives to break down stereotypes. Another geek-a-betic uses comic book analogies to explain his experience with the disease.

April Blackwell (AKA “Nerdy April”) is an actual rocket scientist for NASA. She is very active on her Instagram account. She also writes about her experiences regularly. I reached out to April to get recommendations for other T1D geeks to follow. These nerds include…
- @nerdabetic
- @marsala90 (he is a T1D pilot)
- @erniecam (a friend of hers in real life)
- @nerdscanfight
April also shared a quote, and I think it can apply to all hardships and barriers we have all faced this year:
I really follow a Latin phrase we use in mission control, “ad astra per aspera,” which means “a rough road leads to the stars.” Type 1 diabetes has only shifted my dream. It’s no longer just to be an astronaut, now it’s to be the first T1D in space!
Thank you, April, for taking the time to share!
If you want to learn more about Diabetes, November is Diabetes Awareness Month. You can read more on the Junior Diabetes Research Foundation website or Beyond Type 1.




